

The main problem with a herniated disc is usually, that the disc exerts pressure on a nerve (more precise: nerve root). The work of a neurologist is to examine nerve function. With additional training in a certain subspecialist area of neurology (clinical neurophysiology, NCS, EMG), the function of nerves can be measured precisely. This is very important information to decide on the adequate therapy. Here, a close collaboration between specialists of the spine, orthopedic surgeons and neurologists is often very helpful to decide on the best treatment.
This interdisciplinary collaboration is especially useful in the following situations:
- if “nerve-symptoms” occur – possible symptoms of a “pinched nerve” at the level of the cervical or lumbar spine are: pain is not restricted to neck or lower back but radiates into arm or leg; possibly further symptoms, such as sensation of tingling, „pins and needles“, numbness, muscle weakness, etc.
- if the question has been raised, whether for instance „falling asleep“ of the hands is actually caused on the level of the cervical spine or might be caused as well by a pinched nerve in the further course of the arm (in this situation, of course, the therapeutic approach is quite different)
- if the results of the MRI suggest, that a herniated disc is exerting pressure on a nerve root
- if the MRI shows a „big“ disc herniation
- in case the MRI shows not only one but several disc herniations, possibly causing narrow passages of nerve roots, and now the question arises, which level causes the symptoms and should be targeted therapeutically – (The main advantage of modern therapeutic approaches is an oftentimes quite astonishing accuracy in the range of millimeters. The more accurate the therapy can be targeted though, the more accurate should the symptom-provoking process be localized beforehand. Targeting therapy very precise in the range of millimeters, but at the wrong spot, will not help)
- if MRI suggests, that a nerve damage might occur and the risk of persistent neurological deficits exists
- if important therapy decisions have to be made: is an operation necessary? Is there impending nerve damage?

By means of the neurological examination, it can be distinguished, whether a nerve root is „only“ irritated or actually damaged. In my eyes, this is by far the most important criterion to decide, whether an operation is necessary or not.
Because disc herniations are frequently found on MRI (even in totally asymptomatic people), seeing a disc herniation on MRI does not mean necessarily, that this actually causes the symptoms! There are quite a number of other possible “neurological causes” that can mimick the symptoms of a disc herniation. If the symptoms are not caused by a herniated disc, the best spinal surgery will not remove the cause of the symptoms. To clarify these questions beforehand is another important aspect of the neurological examination.
So why again should I see a neurologist in the case of a disc herniation? I do see the role of the neurologist as an important part of the whole team; the neurological examination in the beginning is mainly for diagnostic purposes, to answer the following questions:
Are my symptoms actually caused by changes of the spine? Is a nerve root affected? Which one? Is the nerve root irritated or damaged? Is there a measurable deficit in nerve function? Am I at risk for persistent neurological deficits? Is an operation necessary? Is there a reasonable time-window for non-surgical therapies? etc.
Most important is a good teamplay (of course only if you want this; some people come for a second opinion only or are under care of a multi professional spine team and only come for neurological evaluation), which means discussion of findings and therapeutic approaches with the whole team involved in diagnosis and treatment (general practitioner, orthopedist, neurosurgeon, spine specialist, physiotherapist, osteopath, etc).
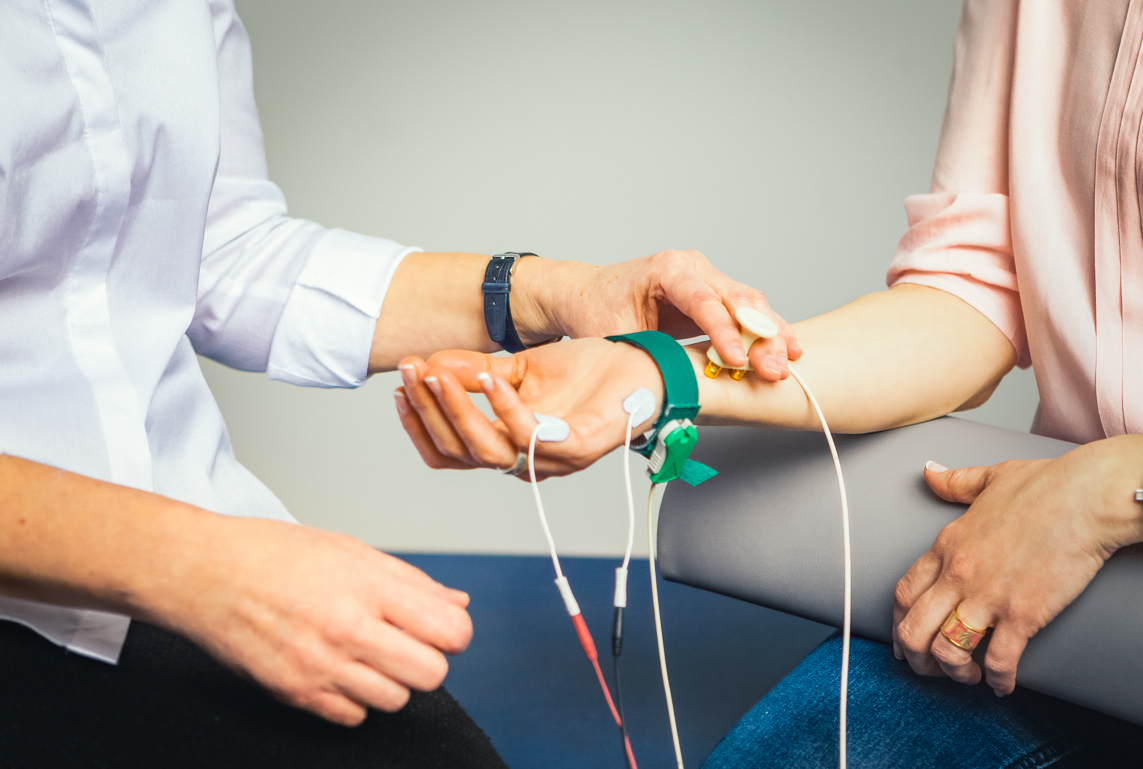
Whether or not the symptoms are caused by carpal tunnel, another nerve entrapment syndrome (“pinched nerve”), a problem of the cervical spine or a disturbance of blood supply –it is very important to accurately examine for the actual cause of the symptoms. Only if the cause of the symptoms has been defined precisely, an effective therapy can be started.
A subspecialty area of neurology is the exact measurement of nerve function using clinical neurophysiology (NCS = nerve conduction studies, EMG = electromyography). As a neurologist trained and specialized in clinical neurophysiology, I have special expertise in testing nerve function. Using NCS and EMG, the function of the nerves or nerve roots can be very accurately measured. In the case of the hands “falling asleep” this is very useful, in order to answer the following questions:
Are my symptoms caused by a “pinched nerve”? If yes, which nerve and where exactly? Is it carpal tunnel? Another nerve compression? Or is the cervical spine actually causing my symptoms? In the case of a carpal tunnel syndrome: is there a deficit of nerve conduction („nerve damage“)? Can the nerve damage be graduated as mild, moderate or severe? That is: is it “dangerous”? Is there a risk of persisting neurological deficits? Should I opt for surgery? Is there a reasonable time-window for non-surgical therapies? Which therapeutic options exist? etc.
So, why again should I go to see a neurologist if my hands are „falling asleep“?
I do think, the question is neither “who does it best?”, nor “who knows it all?”. The question rather is, who can contribute important puzzle pieces in order to see the whole picture at the end. To see “the whole picture” a good teamplay with different medical specialists (general practitioner, hand surgeon, orthopedist, neurosurgeon, spine specialist, physiotherapist, osteopath, etc) is most important.

- repeatedly “falling asleep” of hands or feet
- tingling, “pins and needles” of arms or legs
- numbness of arms or legs
- other sensory disturbances or paresthesias of arms or legs
- pain, especially if going along with other sensations (tingling, pins and needles, burning sensations, „like an open wound“, „like a sunburn“, etc).
- suspected pressure palsy
- muscle weakness of arms or legs
- carpal tunnel syndrome
- ulnar neuropathy at the elbow (UNE)
- Sulcus ulnaris syndrome (SUS)
- Cubital tunnel syndrome
- Loge de Guyon Syndrom
- Pressure palsy of the radial nerve
- “wrist drop”
- “Saturday night palsy”
- “Honeymonn palsy”
- Thoracic outlet Syndrome (TOS)
- Meralgia paresthetica
- Pressure palsy of the peroneal nerve
- “foot drop”
- “strawberry pickers palsy”
- “slimmers palsy”
- Tarsal tunnel syndrome
- Muscle weakness, muscle pain, muscle ache
- Muscle cramps if not reponsive to magnesium are frequently due to neurological causes
- myopathy, diseases of muscles
- Myasthenia gravis
- Lambert Eaton Syndrome
- Amyotrophic lateral sclerosis or motor neuron disease
- Tremor
- Polyneuropathy
- Due to diabetes
- Due to other causes
- Subacute comined degeneration (e.g. due to B12-deficiency)
- Disc herniation
- cervical root problems
- lumbar root lesions
- Spinal stenosis
- cervical spondylosis
- spondylotic radiculo-myelopathy
- cervical myelopathy
- spinal intermittent claudication




American Academy of Neurology (AAN)
In our office we offer evaluation and treatment services for athletes experiencing neurological issues related to sports injuries such as:
• Evaluation and treatment of pain syndromes affecting athletic performance.
Patients often come with one of the following questions: Is the pain due to a nerve problem? Is it because of a „pinched nerve“? what to do?
• Evaluation and treatment of athletes who have suffered concussions or mild traumatic brain injury (mTBI).
A neurological examination and counseling is aimned at answering the following questions: Do I have suffered a concussion? How to manage this condition? When can I return to play? The aim is to help get athletes back on the playing field timely and safely.
• Muscular issues such as fatigue, cramps and poor endurance can be of neurological origin as well. To sort this out, we offer specialized diagnostic examinations and treatment for nerves and muscles.


If for instance pain is due to a nerve problem, this changes the management. Thus, the first question to the sports neurologist is commonly: is there a neurogenic origin of pain? To sort this out, we offer specialized and innovative diagnostic examinations and treatment for nerves and muscles. For more information about our diagnostic approach see the section diagnostics.
Why should I go to a neurologist?
A doctor caring about peripheral nerve injuries or neurogenic pain in sports needs a sound knowledge of neuroanatomy and neurophysiology, as well as a profound knowledge of possible neurological symptoms and signs. Furthermore biomechanical risk factors associated with various sports have to be considered.
In our office we offer specialized diagnostic procedures in order to evaluate nerve function. Besides neurophysiological testing of nerve function (see section on NCS and EMG), we are using nerve ultrasound to actually see the nerves and find out what is wrong (see section on nerve ultrasound). nerve ultrasound also allows dynamic testing, that is visualizing nerves during movements, because sometimes a nerve entrapment occurs only in a certain limb position.
Proper recognition can prevent unnecessary diagnostic testing and delay in diagnosis. The sooner appropriate treatment can be installed, the better is the prognosis.

Concussion is a type of brain injur which results in impairment of normal brain function. It occurs when the brain is rocked back and forth or twisted inside the skull. A concussion does not alter brain structure and is not a brain hemorrhage (that means MRI oft the brain and skull is usually normal) – but it changes how the brain normally functions.
Which symptoms can be caused by a concussion?
Thus a variety of symptoms can be caused by a concussion. Symptoms include headache, sensitivity to light or noise, nausea, dizziness, troubles with balance (vestibular dysfunction), problems with attention, troubles with concentration or memory (cognitive symptoms), foggy thinking, as well as fatigue, feeling sleepy or groggy, sleep disturbances, mood changes.
I have not lost consciousness, can I still have a concussion?
Yes, you can have a concussion without losing consciousness. In fact, very few people lose consciousness when they sustain a concussion.
Prognosis
Most concussions result in full recovery. Duration of symptoms can be quite variable and symptoms may last from a few days to several months, sometimes even longer. These symptoms should be recognized and treated properly in order to ensure a good and rapid recovery and to prevent complications. So dont hesitate to seek specialiced medical advice or to seek a second opinion if in doubt.
What is the main risk?
One of the main is the increased risk of a second head injury (as long as symptoms are not completely recovered). The second head injury is trhen usually associated with higher severity of symptoms and inreased recreation time. An athlete who sustains concussion is 4-6 times more likely to sustain a second concussion. This is probalbly due to decreased speed of neural information processing, resulting in slower reaction times, impaired concentration or balance problems.
Why concussion testing?
Complete healing is key to reduce the risk that a first head injury can cause a second concussion. This is why a a stepweise return-to-play or return-to-school is recommended. This should be individually adapted, based on the results of neurocognitive and neurovestibuar/neuroophthalmological testing.

Is the brain an important organ in sports?
The human brain is an incredible fast and complex organ, even modern computers fall way short to reach the brains capacity of signal processing. A concussion usually means decreased speed of neural information processing, resulting in slower reaction times, impaired concentration or balance problems. In many sports, decisions based upon complex integration of different informations (experience, assumptins, visual, acoustic, vestibular und other informations) are made within milliseconds, usually there is not time to think. In this sense, a lot of sport situations rely on a 100% brain health that makes all the difference.
Why going to a neurologist?
In the days following a concussion you should see a concussion expert. Ideally this should be a physician specializing in brain disorders. Most of the concussin symptoms are within the neurological spectrum. Headache, dizziness, impaired concentration… A neurologist is trained to recognize and manage these symptoms. Before return to play – similar for return to school and return to work – the symptoms must have cleared completely.
What happens during a concussion consultation?
A specialized concussion consultancy inludes a neurological assessment, special evaluation of balance, vestibular system, visual system and tests of cognitive function, such as attention, concentration, and memory. More tests such as brain imaging (MRI) or other tests might be ordered, depending on the individual symptoms. Always the focus is on full and safe return to play. According to test results, counseling on therapy (if needed) and return to management is given. These test results are important information to assist in decisions regarding return to work, return to school or return to play.
What is baseline testing?
Baseline testing (pre-season testing) is offered to all sport athletes at risk for concussions. After a concussion, ideally test results can be compared to test results performed at the beginning of the season, the so called baseline test, when the player was well.
This ensures, that a normal comparison fort he individual athlete is available should a concussion occur. The test score should be comparable to baseline before returning to exercise.
What Sports or other recreational activities are particularly associated with risk for concussion?
Bicycling, Football, Playground, Basketball, Soccer, All-terrain vehicle riding, Skateboarding, Swimming, Hockey, Miscellaneous ball games
Is concussion only important in sports?
Of course, Concussions are not limited to sports. They can result as well from other injuries, such a s falling, slipping on ice, bicycle accident, whiplash injury, etc.
Here you can make an appointment for a diagnostic.
Do not hesitate to contact us.
Phone 030 23 54 55 45


